Brain Tumor
On this page, I will try to explain the details about the brain tumor, its causes, symptoms, types, diagnosis, treatment methods, brain tumor surgery and its aftermath.I wish you all healthy days.
What is a Brain Tumor?
Brain tumor is the formation of clinical symptoms when abnormal cells in the brain multiply and have a mass effect on the brain in the region where they are located.As it is known, cells are the simplest structural and functional units in man.In a healthy person, new cells are made only to replace them with aged or damaged cells.However, when new cells are made without the need and this process is accompanied by abnormal proliferation, they form a mass in the brain, and this mass is called brain cancer in medicine among the people.The tumors that form may compress the brain tissue or spread widely within the tissue.In addition, brain tumors can cause an increase in intracranial pressure by slowing the flow of cerebrospinal fluid in the central nervous system or completely stopping the flow.
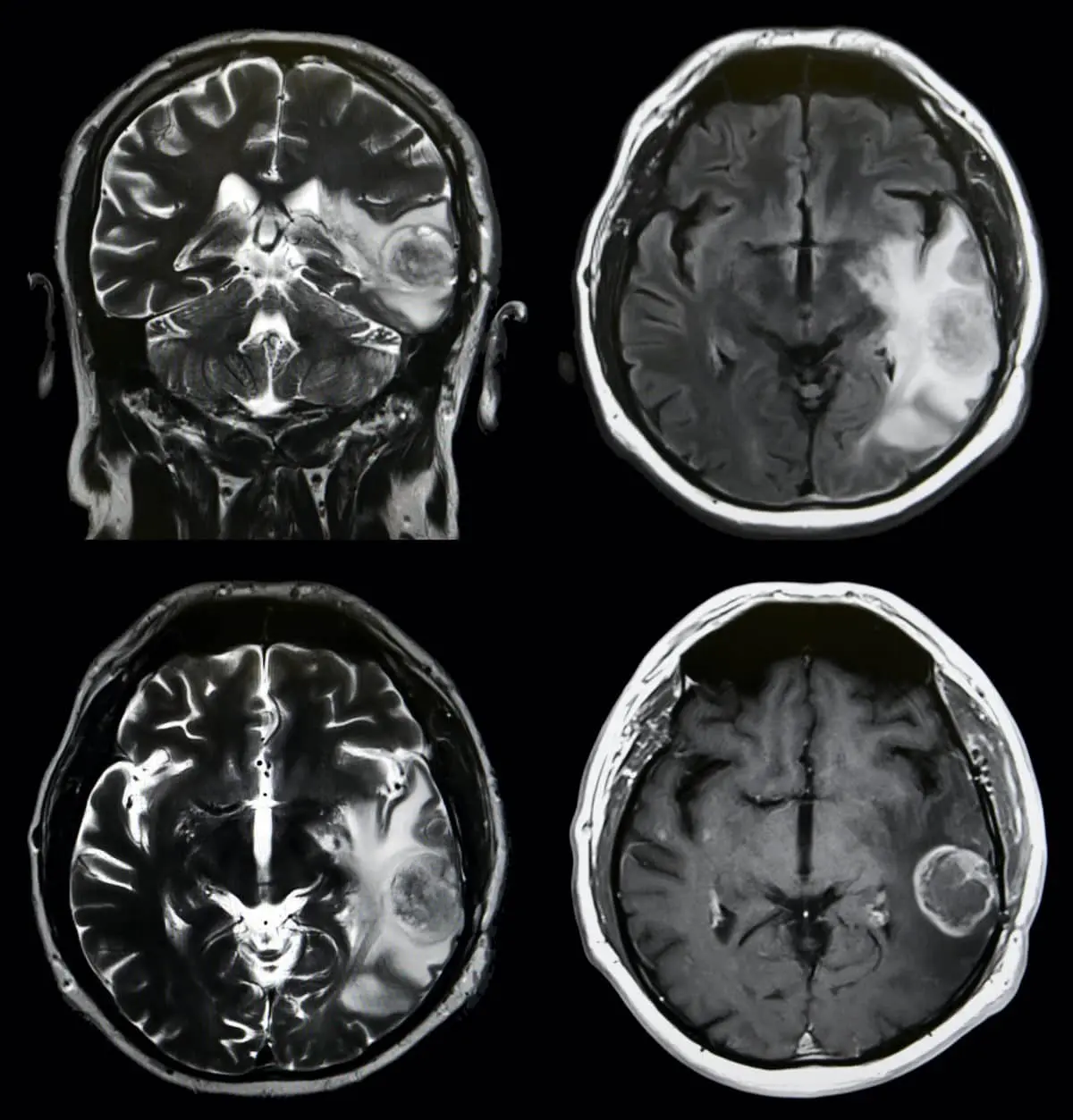
Why Does a Brain Tumor Occur?
A brain tumor is caused by abnormal growth of brain tissue.If the tumor originated from the brain, it is called a primary brain tumor.Primary brain tumors are also classified as benign and malignant.The prevalence of brain tumors in the community varies between 3-5 in 100000 people.
What Causes Brain Tumor?
A lot of studies are being done on this subject. The exact reason to blame is as little as none.However, it is known that some factors play a more common role in patients with brain tumors.These factors can be listed as male gender, white race, over 65 years of age.Radiation exposure is known to increase the risk of brain tumors from radiation therapy.Some brain tumors also show familial transmission.Some raw materials used in the plastic and textile industry have also been identified as risk factors.
Brain Tumors Are More Common in Who?
It is more common in men than in the yellow race and women.Benign brain tumors called meningiomas are more common in women.Brain tumor can be seen in all age ranges.Malignant ones are mostly seen in children and over 60 years of age, while benign brain tumors are more common in the remaining age ranges.
Types of Brain Tumors
In general, brain tumors are divided into 3 as benign, malignant and metastatic brain tumors.
What Are Benign Brain Tumors?
Benign brain tumors are not cancerous.They grow slowly, often have clear boundaries.Benign tumors can also be dangerous.They can compress or damage critical functioning parts of the brain.Sometimes, benign brain tumors can be found in areas that are very difficult to reach or have high complication rates when surgery is performed in that area and can be life-threatening.They also cause serious loss of function in the areas where they are damaged.Benign brain tumors are usually removed by surgical treatment.They are less likely to relapse. Very rarely, benign brain tumors turn into malignant (malignant) brain tumors.
What Are Malignant Brain Tumors?
Malignant brain tumors are cancerous.So there are cancer cells in the tumor tissue.They typically grow quickly. They spread to healthy surrounding brain tissue.These tumors pose a serious life-threatening condition.They spread to the spinal cord very rarely.
What Are The Most Common Metastatic (secondary) Brain Tumors?
The cancers that have spread the most to the brain are:
• Breast cancer
• Colon cancer
• Kidney cancer
• Lung cancer
• Skin cancer (melanoma)
Metastatic brain tumors spread through the blood.These tumors are always malignant tumors.As a result of the spread of the tumor through the blood from the primary cancerous tissue, it is located in the hemispheres of the brain or in the cerebellum.Cancer can also spread to the spine.Those that spread to the spine are also called metastatic spinal tumors.Metastatic brain tumors grow rapidly and damage nearby brain tissue.In some patients, metastatic focus may be detected in more than one area of the brain. Some metastatic brain tumors metastasize to the brain years after the detection of a primary cancer located in another organ.
But most brain metastases appear to settle in the brain tissue before the detection of the primary tumor.In some patients, although metastases are detected in the brain, there is no primary tumor located in another organ.Treatment pathways for metastatic brain or spine tumors include:
• Surgery and/or radiosurgery
• Radiotherapy
• Chemotherapy
Why Are Child Brain Tumors Different From Adults?
Brain tumors in children develop from different cell groups and from different parts of the brain than adults.Childhood brain tumors can be recognized earlier than adults.This is because the signs and symptoms are more pronounced in children and the close and attentive follow-up of their parents.Signs and symptoms may be related to memory, learning, hearing, vision, smell or affect.In brain tumors in children;
• The same type of tumor gives different symptoms than the adult.
• Treatment may vary according to adult.
• In children, the transformation of a low-stage malignant (malignant) tumor into a high-grade tumor is less frequent.
• The chance of survival is higher than in adults.Brain tumors are the second most common type of cancer in children.Brain tumors constitute 21% of all children’s cancers.Although brain tumors can be seen in children of all ages, the under-7 age period is the riskier period.Tumors located in the spinal cord can also be seen in childhood.However, their incidence rate is less than brain tumors.

What Are the Most Common Types of Brain Tumors in Childhood?
The most common tumor is gliomas.According to the cell from which they originate, they are classified with different names according to the location.Example of naming according to its location: To give an example of the brain stem glioma, the cell from which it originates, primitive neuroectodermal tumors can be mentioned.When these tumors are located in the cerebellum, they are called medulloblastomas and grow rapidly, blocking the flow of cerebrospinal fluid, causing increased pressure inside the head.Medulloblastoma can spread to other parts of the brain and the spinal cord.
What Are the Symptoms of a Brain Tumor?
Different parts of the brain control different functions.Therefore, it differs in signs and symptoms.Tumor size, location and the rate of expansion in size are the most important factors in the emergence of signs and symptoms.Signs and symptoms that usually occur (one or more of these findings may coexist);
Headache Seizures and fainting Difficulty thinking,
speaking, and finding words and/or slowing down
Personality and behavior changes
Weakness in one part or one half of the body
Loss of balance, dizziness, dizziness
Hearing loss
Visual impairments
Confusion and disorientation
Memory loss
Brain Tumor Diagnosis Stage
During the diagnosis phase, listening to the patient's history and subsequent neurological examination are very important.In line with the information obtained here, radiological examination and electrophysiological examinations are requested to diagnose the patient.
What are Radiological Examination Techniques?
How is Neurological Examination Performed?
When you go to the neurosurgeon for examination, first of all, you and / or your relatives are asked what your complaint or complaints are.Then, how long these complaints have been, their duration and other details are questioned.A detailed neurological examination will then be performed.In neurological examination, vision, hearing, strength, sensation, balance, coordination, reflexes, thinking ability and memory, recall functions are evaluated.As a result of this evaluation, if radiological examination is required, you are told which examinations will be performed and the reasons for them.
Angiogram
Angiogram is a kind of X-ray examination method.With this examination, the arteries and veins of the brain are shown.You are given an injection of contrast media and then the vascularization of the brain is displayed.Thus, abnormalities in the vascularization structure (such as aneurysm-bubble in the brain, arteriovenous malformation-vascular ball) are detected.
Computerized Brain Tomography
In computed brain tomography, the examination is performed with the help of X-ray.In the examination, 3D imaging of the brain is obtained by using the X-ray at different angles.These images are converted into images on the computer by means of a special software and abnormalities or tumors in the brain are detected.Computed brain tomography is especially useful in the diagnosis of brain tumors that are adjacent to bone tissue or have caused damage to bone tissue.With this diagnostic tool, tissue damage, bleeding, bone-tissue calcifications can also be detected.Computed brain tomography is used in daily clinical use, mostly as the first choice diagnostic tool in emergency situations.
Magnetic Resonance Imaging
It is one of the diagnostic methods that best visualizes brain tissue.In this diagnostic method, magnetic waves and radio waves are used instead of X-rays.It is a diagnostic method that displays brain tissue much better than computed brain tomography.In recent years, it has become one of the indispensable diagnostic tools of neurosurgeons.With magnetic resonance imaging, it is possible to take lateral vertical, anterior vertical and horizontal cross-sectional images of brain tissue and to visualize the relationship between tumoral formation and surrounding tissues.In some cases, patients may need to be given contrast media and additional imaging may be required.
Magnetic Resonance Spectroscopy
This diagnostic method is also part of the magnetic resonance imaging method.It has very similar aspects to magnetic resonance imaging.Through a special software, biochemical changes belonging to a determined region in the brain can be detected.With magnetic resonance imaging, it is possible to obtain information that helps diagnose infection, stroke, Alzheimer's Disease, multiple sclerosis, scar formation after radiation and tumors.
Diffusion Tensor Imaging
In this imaging method, the water flow in the white matter pathways of the brain is measured.Here, the image of the structural state of the brain at that moment is determined.In later periods, it is possible to make comparisons between this image and new images.The importance of this imaging technique is to show the relationship between tumor and white matter structure and to contribute to the surgeon preventing damage to these pathways as much as possible in surgery.
Functional Magnetic Resonance Imaging
Functional magnetic resonance imaging enables the detection of specially functioning areas of the brain.For example, the speech center, the display of the regions of our body that provide motor movements.The operation of this technique is like standard magnetic resonance imaging.However, it provides a more advanced level of information by providing the measurement of the amount of oxygen in the blood vessels and the small changes in them.These changes in the amount of oxygen indicate which areas of the organ are functional.For example, when the relationship between the speech center and a tumor close to it needs to be detailed; The patient reads what is written on a page in his hand during the shooting, and at the same time, the speech center is detected in the imaging made using special software.The neighborly relationship of the tumor with this area is determined.The neurosurgeon also has the chance to plan the surgical intervention to be performed in this area in more detail.
Biopsy - Tissue Sample Analysis Explained
Biopsy is a diagnostic method that gives extremely important information to the neurosurgeon as a result of the evaluation of the tumor tissue sampled during surgery by pathologists.If this tissue sample is taken during surgery, it is called an open biopsy.If the tumor is in a part of the brain that performs very critical functions, or if there is a possibility of serious damage during the removal of the tumor from here, or if the patient has health problems that cannot complete the operation process, another diagnostic biopsy method is stereotactic brain biopsy.In this method, the location of the tumor is determined in 3D by attaching a special head to the patient and with the help of a computer and a biopsy is taken.The biopsy taken is evaluated by the pathologist and the diagnosis is made.After this process, the neurosurgeon can talk more clearly about the course of the disease and plan additional treatments or if a second surgery is required.Therefore, pathological diagnosis is of vital importance both for the patient and for the neurosurgeon.
Positron Emission Tomography
With this examination, changes such as growth in the cells are detected.Very low doses of radioactive glucose are injected into patients. Depending on the stage of the tumor, the tumor absorbs some radioactive glucose compared to the surrounding normal tissues and the tumor tissue is detected by these radionuclear imaging software.Positron emission tomography gives a rough idea of the severity of the tumor growing.
Cerebrospinal Fluid Examination
Under local anesthesia, cerebrospinal fluid is taken by entering the lumbar region with a needle.Biochemical and pathological examinations are performed on this removed fluid.After resting for 1-3 hours, the patient is sent home.
Brain Tumor Treatment, Brain Tumor Surgery and Preparation Process
The diagnosis of a brain tumor is a difficult period for every patient and his/her relatives in terms of their feelings. In this period, patients want to get as much information about their diseases as possible, and even make decisions by having this information verified by several neurosurgeons. There will also be times when the patient who decides on the surgery is undecided in choosing his physician. The support of the patient's family is very important in this process of indecision. In the case of a patient whose diagnosis is confirmed, you will be given detailed information by me in the light of the patient's history, examination and imaging methods findings. The information to be given includes the location and surgical difficulty of the tumor, the possibility of good or malignant tumor as a preliminary estimate in the light of imaging methods, the planned surgical method, the duration of the operation, the postoperative intensive care period, the total hospital stay, the rate of affecting the quality of life of the surgery, surgical and vital risks, the financial dimension of the operation. After deciding on your surgery, we will need to prepare the examinations including the necessary laboratory and imaging methods before the operation and send you to the anesthesiology department and get approval.
Following the approval, the last preoperative stage is to decide on the day of surgery together.If the patient does not have an urgent clinical picture or a systemic disease or general condition disorder that needs to be corrected in advance, then it will usually be sufficient for our patient to be hospitalized in the morning of surgery.Treatment options are determined according to the type of tumor, its location and the analysis of the treatment results in the literature.But in general, the options are surgical treatment, radiation therapy and chemotherapy.In most of the brain tumors, surgical intervention is the treatment method that is prioritized.However, it may not be possible to reach and treat some tumors localized in the brain stem surgically.In this case, the option may be radiotherapy.

How Is Craniotomy (opening the skull) performed in the Treatment of Brain Tumors?
Brain tumor surgery is performed under general anesthesia.First, the hair in the area to be operated is cut. A spiked cap is worn to give the patient's head a position and to prevent the head from playing in the operation.Then the surgical site is wiped with an antiseptic solution. Then the edge of the surgical site is covered with sterile surgical dressings.Following the full preparation of other surgical equipment, the craniotomy procedure is started.An incision is made on the skin at the previously drawn boundaries and the tissues called skin, subcutaneous, galea, periosteum are stripped over the bone and a bone fragment of the planned size in the skull is removed with a special drill.The removed part is stored to close again at the end of brain tumor surgery.After the bone part is removed, the tissue that comes to us is the brain membrane layer that surrounds the brain.After this membrane is opened properly, the brain tissue is reached.In brain tumor surgery, if the surgical site is in a deep and important area of the brain, a computer-aided system called navigation can also be used to cause the least damage to the brain tissue.The operation is performed under a microscope. The area of brain tissue other than the place where the incision will be made in the brain tissue is protected with soft cottons and then a small incision is applied from the planned place.In brain tumor surgery, a corridor that will be least risky and least damaging the brain tissue is selected and the tumor tissue is reached.After this point, the tumor is removed by appropriate surgical technique.In the process of tumor removal, the most modern technology is used in terms of operating room conditions and surgical instruments.The most important step in brain tumor surgery before termination of surgery is very careful bleeding control.After this stage is completed, the dura layer called the cerebral membrane is closed and the bone fragment removed at the beginning of the surgery is replaced and fixed to the skull.Then, the periosteum, galea, subcutaneous and skin covering the bone are closed and the operation is terminated.Some tumors can destroy the brain membrane and bone tissue, in which case the brain membrane and bone can be removed and then repaired by using biologically suitable synthetic tissues.In head back pit surgeries, sometimes the bone tissue at the operation site is removed in smaller pieces and then this place is repaired by using the synthetic tissues I mentioned above and cosmetically corrected that area.
Your Questions After Brain Tumor Surgery
After the brain tumor surgery, you will first be taken to the patient wake-up unit of the anesthesia department and then to the intensive care unit.The intensive care process, which is the most curious and perhaps feared place as a patient, is more comfortable and bearable with both the spread of technological facilities and the support of trained intensive care personnel.The patient, who is taken to intensive care after brain tumor surgery, will try to understand his naturally occurring condition when he wakes up.He is in the position of a patient with serum attached to his arm, a urine catheter, cables attached to monitor the arrangement of his heart from the chest area, the place where the surgery was performed on his head was closed with dressing material, another cable measuring the blood oxygen status was inserted in one of the fingers.Since it is necessary to check the patient's consciousness at frequent intervals after brain tumor surgery, the patient will be awakened at frequent intervals, especially in the first night.Therefore, the patient will spend the first night partially sleepless.In addition, the patient should be calm and avoid excessive movements when trying to understand his own condition.Such clear information of our patients before surgery is a prerequisite for the intensive care period to be more comfortable after brain tumor surgery.After the conscious patient spends the first night in the intensive care unit, the appropriate nutrition regimen is started and the patient is executed.The patient is checked for the last time before the operation site is taken to the patient room by taking the control brain tomography on the 1st day.Usually the patient is taken to his room on the floor after the second day.The patient who stays in his room for an average of 3-5 days is discharged.The sutures of the discharged patient are removed on the 8-10th day.The patient will need to use certain medications when sending home. For this, the patient is given a written note stating how to use his medications and is ensured to use his medicines regularly.
Complications After Brain Tumor Surgery
The most common complaint in the patient who wakes up after brain tumor surgery is headache, weakness and fatigue.The headache may last for several days. The patient's malaise process may last longer.One of the most important stages when terminating brain tumor surgery is to ensure that there is absolutely no bleeding in the brain tissue.However, despite all the care and attention, patients may need to be operated again under emergency conditions due to postoperative bleeding.The problem of infection may occur at the site of the wound, in the bone tissue that makes up the skull or in the brain tissue.In this case, drug treatment and/or surgical treatment may be required.Another problem seen after brain tumor surgery is brain edema.In the simplest terms, it is the increase in the water content of the cells in the brain tissue.The problem of brain edema can be solved by using drugs that mostly contain steroids (cortisone) and/or a group of drugs that serve to reduce brain cell water content.After brain tumor surgery, sometimes an increase in intracranial pressure is seen as a result of the disruption of the circulation of the cerebrospinal fluid in the water sacs in the brain.
In this case, the intracranial pressure is reduced by directing the cerebrospinal juice into an outer bag or into the abdominal cavity with a catheter placed in the abdominal cavity with the tube placed in the cerebral water sac.Depending on the location, size, surgical method and path used in brain tumor surgery, sometimes patients may have problems in losing strength in the arms or legs, thinking, seeing and speaking, evaluating and judging events.The risks of these problems can be partially predicted by preoperative imaging methods.Most of these problems decrease or disappear over time after brain tumor surgery.But some disorders can be permanent. Patients may have seizures (epileptic attacks) with the effect of the tumor before the operation and with the effect of the surgery after the operation.In this case, the patient is started from one of the drugs used in epilepsy patients.The patient is ensured to use this drug regularly.Because these drugs must be at a certain blood level in order to be effective.The level of medication that prevents epilepsy attacks after brain tumor surgery should be checked after 20 days of use and dose adjustment should be made if necessary.In addition, many epileptic attack prevention drugs have the potential to have a negative effect on the liver and blood table.For this reason, the patient should be checked by performing whole blood and liver function tests every 3 months.In addition, patients who have seizures should pay special attention in some situations in their lives (such as driving, swimming alone in the sea) and should not endanger their own lives as well as the lives of other individuals.

Success Rate in Brain Tumor Surgery
In brain and nerve surgery, brain tumors with various characteristics are encountered.Success rates in brain tumor surgery vary considerably with whether the tumor is benign or malignant, the location of the tumor in the brain, the experience of the surgeon, and the additional treatment requirements to be applied after surgery.If there is a brain tumor located in a benign area of the brain that is not difficult to localize, if the experience of the surgeon is sufficient, the probability of complete removal of the tumor is very high and there is often no need for another treatment option.Radiosurgery applications should be considered as an option in benign brain tumors that cannot be completely removed.In malignant brain tumors, the tumor may not be completely removed and then radiotherapy, chemotherapy, radiotherapy or radiosurgery may be needed.
Radiotherapy, Radiosurgery and Chemotherapy in Brain Tumors
Radiotherapy (radiation therapy) after brain tumor surgery is another treatment method that is widely used in brain surgery practice.Sometimes, radiotherapy can be applied without surgery because the location of the tumor is located in a place that may cause very serious problems with surgical treatment or the general condition of the patient is not suitable for surgery.In radiotherapy, the therapeutic beam mass is applied to the area in the brain where the tumor is removed or where part of it is removed and the other part is left in the brain tissue and to the surrounding brain tissue very nearby with computer-aided tools in the post-brain tumor surgery.After radiotherapy, redness, skin sensitivity, hair loss, nausea, vomiting can be seen on the skin.In addition, edema in the brain tissue (increase in the water content of the brain tissue) and the associated increase in intracranial pressure can be observed.Radiotherapy in children is decided only when it is very necessary.Because radiotherapy in children has a very negative effect on growth and development, it also leads to the deterioration of brain cognitive functions (thinking, judging, decision-making, intellectual functions).Therefore, inter-clinic consultations (brain and neurosurgery, radiation oncology, medical oncology, pediatrics) may be more needed in the execution of the treatment plan after brain tumor surgery in children.Radiosurgery applications (gamma knife, cyber knife) are used for tumors that are not suitable for brain tumor surgery and tumors that cannot be completely removed after surgery.It has become very popular in the last 10 years. High-dose radioactive radiation therapy is applied to the tumor area determined by special examination brain MR imaging in a way that does not damage the surrounding tissue.Chemotherapy is a treatment method used to kill cancer cells that are located in the brain tissue or remain after brain tumor surgery.The most important factor determining its use after surgery is the result of the tumor from the pathology department.Sometimes, it is applied to avoid the negative effects of radiotherapy, especially in children, and to give children time until they will be least affected by radiotherapy.Chemotherapy is administered in certain intermittent periods. This application is to ensure that patients are less affected by the negative effects of drugs.The department that plans the chemotherapy process is medical oncology clinics.There are also slow drug-releasing chemotherapy agents that are placed in the space formed after the tumor is removed in the brain tissue. After these are placed at the surgical site, the closure of the surgical site is done by the standard method.The drug kills tumor cells by slowly releasing it and spreading it into the brain tissue.
Other Tests Used in the Diagnosis of Brain Tumors
Certain blood and urine tests are necessary in certain types of brain tumors (such as a pituitary tumor).With these tests, the level of hormones and metabolites in the patient is examined and the results are evaluated together with the results obtained from other radiological diagnostic methods.

Life After Brain Tumor Surgery
When the patients successfully end the brain tumor surgery and are discharged from the hospital, a completely different life will have started for our patient and his family.Among the many factors about how this lifestyle will be and whether additional treatment will be required after this stage; is the pathological diagnosis of the patient.While the pathological result can sometimes be reached immediately with the emergency pathological study (frozen tissue biopsy) applied in the surgeries, the pathological diagnosis can be reached by special pathological staining processes performed in the laboratory 5-8 days after the brain tumor operation.Other factors affecting life after brain tumor surgery are the age of the patient, the preoperative clinical condition, the age of the patient, whether the entire tumor has been removed, whether additional treatment is needed, the adequacy of postoperative cognitive functions and whether additional treatment is required.All these should be evaluated jointly with the support of physicians, patients, patient relatives and, if necessary, psychiatrists, and the patient should be helped at the points where he can get support in social life as well as being the physician who performs the surgery.After brain tumor surgery, stroke (stroke), severe intellectual dysfunction, dependence on the bed can be observed.Although the possibility of these after surgery has always existed; the overall incidence is low.Postoperative death is very rare. If there is a possibility of serious sequelae that can be foreseen before surgery, this should be discussed clearly with the patient and the family.